Heart Murmurs Explained
GLVH
A heart murmur is an abnormal sound heard on auscultation of the chest. They can be variable in intensity/loudness, duration, where within the beats of the heart it occurs, and have multiple possible reasons for existing.
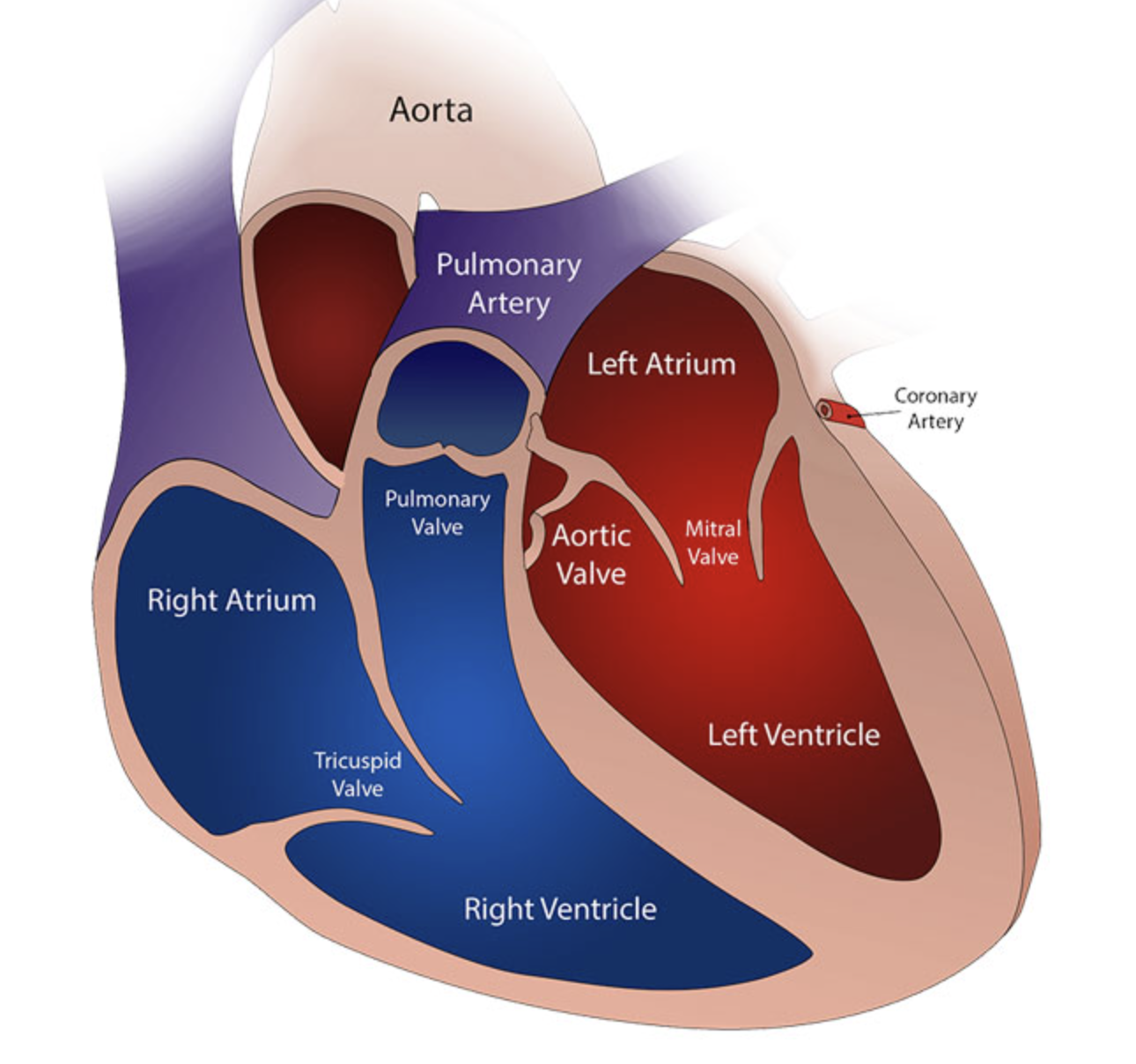
When your veterinarian auscultates the chest (listens with their stethoscope) they are listening for how the heart sounds. The normal heartbeat sounds consist of the first sound (“lub” - closure of the mitral and tricuspid valves) and the second sound (“dub” - closure of the aortic and pulmonic valves). Is it a normal “lub-dub” sound of the valves closing in a normal way? Is the heart beating at a normal rate and rhythm? Does the heart sound muffled or at a “normal” intensity? Do the pulses (often femoral) match the heartbeat? Are they strong, adequate, weak?
Other aspects of assessing the cardiovascular system are observing the colour of your pets mucous membranes (gums are an example) to ensure they are a normal pink colour, and when compressed gently with a finger do they blanche and regain the normal colour within 1-2 seconds. This demonstrates good cardiovascular perfusion and adequate cardiac output. Of course, while we are listening over the chest, we are assessing the lung fields as well to ensure clear respiratory sounds.
If a heart murmur is detected during your pet’s exam it is given a grade between I and VI based on the intensity of it. The louder the sound of the murmur the more severe the heart disease is. The table below outlines how we go about grading a heart murmur.
Intensity Interpretation
Grade I: Very quiet murmur, subtle, often difficult to discern
Grade II: Quiet murmur, sounds are quieter than the normal heart sounds
Grade III: Obvious murmur, as loud as the normal heart sounds
Grade IV: Obvious murmur, louder than the normal heart sounds
Grade V: Very loud murmur with a precordial thrill*
Grade VI: Very loud, precordial thrill, can hear it with stethoscope lifted off the chest wall
*Precordial thrill – when touching the chest with a hand one can feel the vibration of the turbulent blood flow
Next a heart murmur is assessed for when it is present during the cycle of a heartbeat. Is it continuous throughout the whole cycle, is it systolic (only during ventricular contraction) or diastolic (during filling of the ventricles)? Knowing this timing helps narrow the potential cause of the murmur.
Sometimes a murmur can be more specifically isolated over the chest to also help narrow down the diagnosis. This may be isolating it to the left side of the chest versus the right. Whether it is towards the apex of the heart (point where the heart faces the abdomen and sternum) or the base of the heart (top where all the big vessels attach).
More common heart murmur differentials:
· Innocent murmur (stress/physiologic)
· Puppy/kitten murmur (often outgrow this as heart matures by 6 months of age, if not congenital defect likely)
· Valve defect (mitral or tricuspid regurgitation)
· Stenosis/narrowing of the aortic or pulmonic valves
· Ventricular septal defect – hole in the wall between the two ventricles
· Patent ductus arteriosus – necessary opening while in-utero that does not close properly by 10 days old, allows blood to flow from right ventricle/pulmonary artery directly into the aorta instead of to the lungs
· Functional murmur where there is no structural change of the heart but something like anemia/low red blood cell count can cause a murmur due to change in blood viscosity
· Heartworm disease/infection
· Cardiac mass/cancer
What tests can be done to better assess a heart murmur?
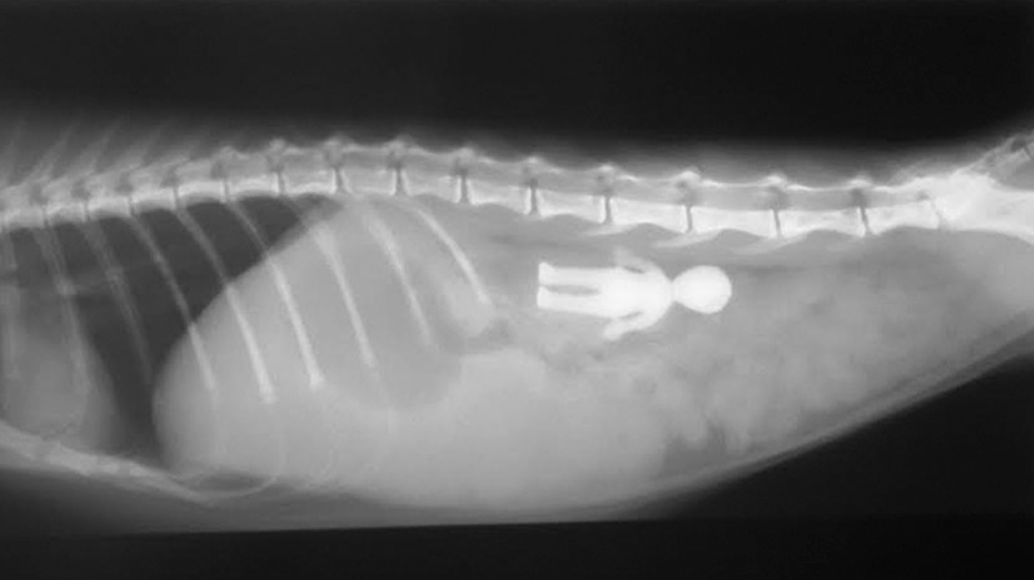
Imaging of the heart is a great way to assess severity of heart disease. A first step is often chest x-rays as most veterinary clinics have this available to them at a reasonable cost. When looking at the x-rays, we are measuring for heart size to see if it is enlarged due to increased work while trying to compensate for the defect. Lungs are also assessed for any fluid build-up, which is seen in cases of congestive heart failure or end-stage heart disease. We also assess the blood vessels to see if they are also enlarged to help determine severity of disease.
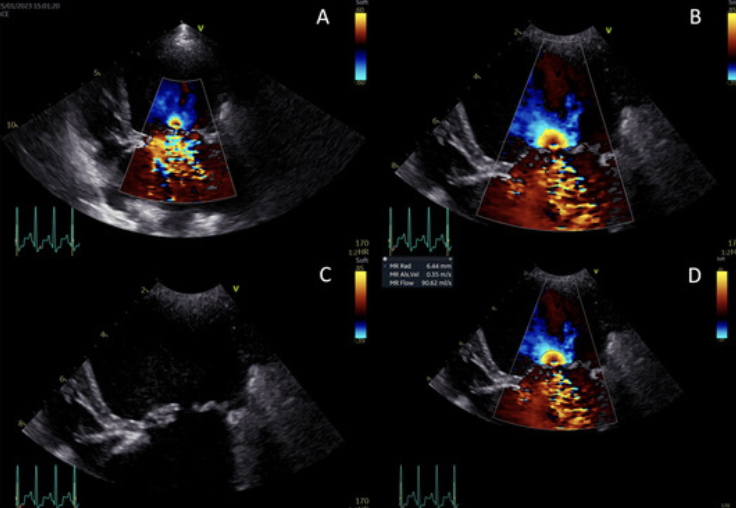
Mitral valve regurgitation on echocardiogram
An excellent modality for imaging the heart is ultrasound to perform an echocardiogram. This allows for actual visualization of the heart beating in real time, where each valve and chamber can be looked at individually and in almost all cases the cause of the heart murmur can be determined. Usually, an echocardiogram is performed by a cardiologist and is something that needs to be referred to by your family veterinarian.
An electrocardiogram (ECG) is another test that is a way to thoroughly assess the hearts electrical activity. It is not always necessary for diagnosing a heart murmur, but is a quick and non-invasive test that provides good information on heart health.
A newer, and quite useful test is a blood test called NT-proBNP that is a marker of heart damage. It only requires a bit of blood work and helps assess the heart from another angle and colours the picture of heart disease a bit clearer. Along the same lines is a test to assess your dog or cat is free of heartworm. If present, they occupy space in the pulmonary arteries and sometimes the heart itself, causing obstruction to normal blood flow.
Levels of heart disease:
A – at risk of heart disease (ie. Breed predisposition)
B – heart disease, no clinical signs
B1 – no chamber enlargement
B2 – enlargement of left atrium/ventricle
C – past or current signs of heart failure
D – end-stage disease
Treatment is generally started at the B2 level of heart disease.
Clinical signs you may see in your pet if they have a heart murmur is exercise intolerance (tires easily), coughing, excessive panting, lethargy, difficulty breathing, and fainting or collapsing.
Can we treat a heart murmur?:
At this point in veterinary medicine most heart murmurs are not surgically corrected except in rare cases. What we can do is provide various medications to help the heart function better despite the cause of the murmur in the majority of cases. Pimobendan is a common first-line drug used to help increase heart contractility. Additional drugs may help through reducing vascular resistance (ACE-inhibitor) by dilating blood vessels so the heart does not have to work so hard to pump blood throughout the circulatory system. In cases where there is fluid building up in the lungs, as seen with heart failure, we can add in diuretics such as Furosemide.
If you pet has been diagnosed with a heart murmur, regular follow-up with your veterinarian is a good idea in order to monitor it for worsening, further clinical signs, heart enlargement and whether treatment is indicated.
Our pets occupy space in our hearts, so let’s take care of theirs,
Dr. Hillary